Perth's Leading Specialist in the Treatment of Varicose Veins
Dr Luke Matar | MBBS, FRANZCR, FACP
High quality, minimally invasive treatments
Your quality of life is our main priority
We specialise in offering the latest technological advances in medical varicose vein treatment. The options we have today are far more advanced than outdated practices such as surgical stripping, which involve lengthy recovery times and often have the veins returning after a few years. Utilising up-to-date methods and continually innovating our processes, we are proud to offer the people of Perth gold-standard treatments which give beautiful long-lasting results with minimal downtime, allowing you to return to daily activities almost immediately.
Discover Our Advanced Varicose Vein Treatments
Non-Invasive, Non-Surgical Solutions
Avoid future complications by seeking treatment today
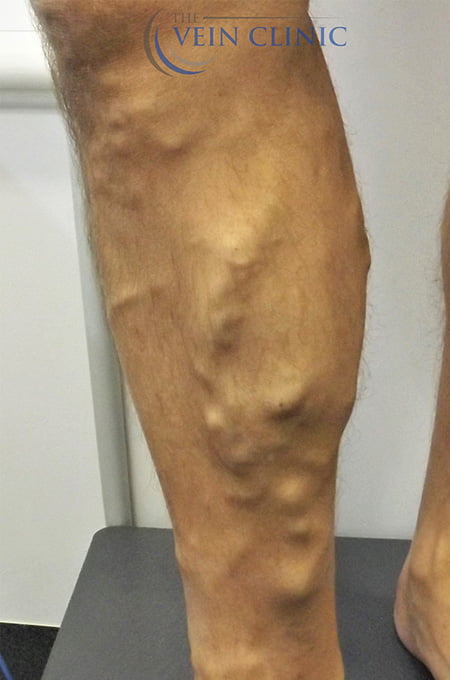
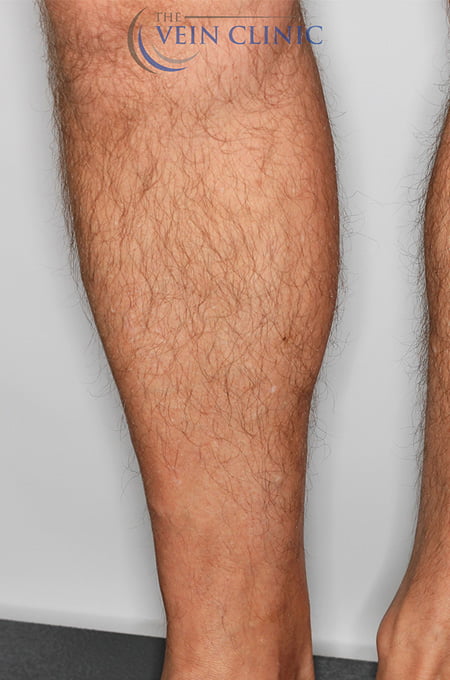
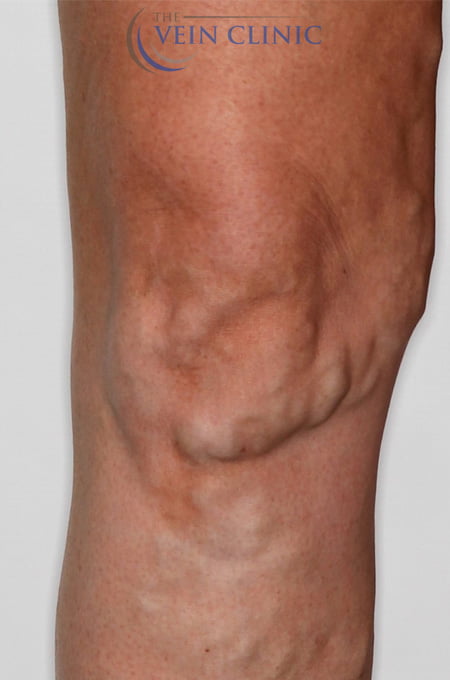
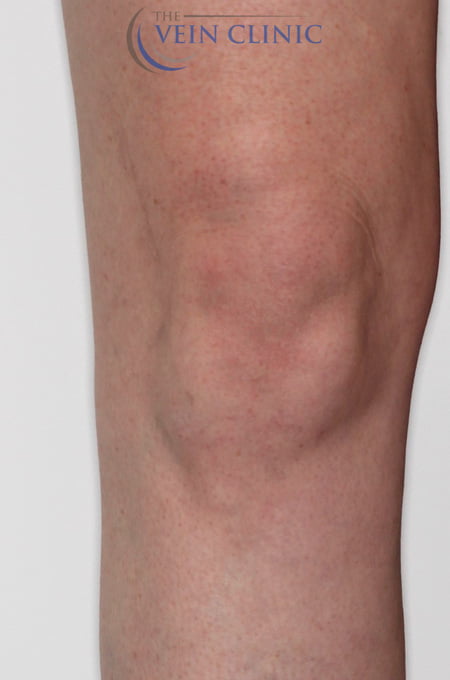
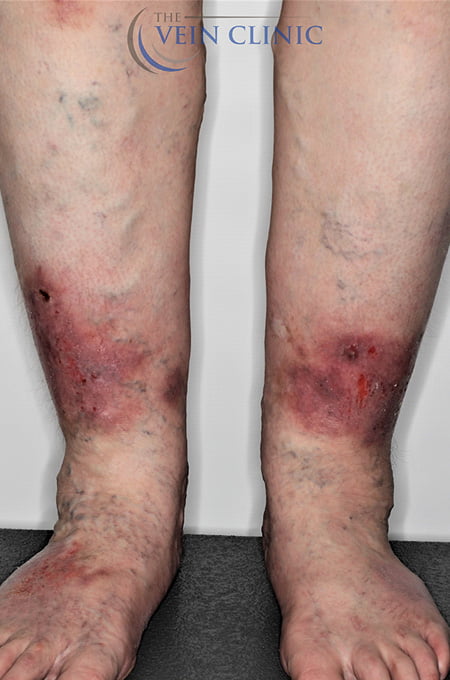
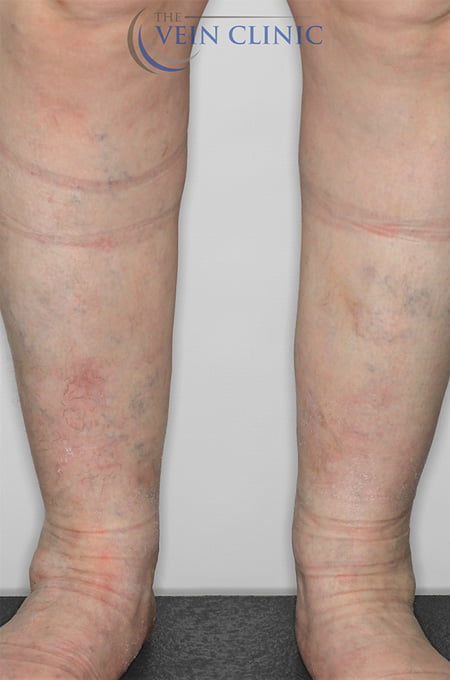
At The Vein Clinic, we focus primarily on medically necessary treatment for the symptoms of venous insufficiency. Daily symptoms such as pain, ache, restlessness, heaviness, or swelling, can often be overlooked when you get used to them over time. However, leaving venous issues untreated can lead to the development of future health issues. Serious complications such as venous ulcers or deep vein thrombosis are severe but do occur. Having interventional treatment early, even if aesthetically your veins might not be “that bad”, can alter the course of your disease progression and save you from experiencing these painful and potentially life-threatening outcomes.
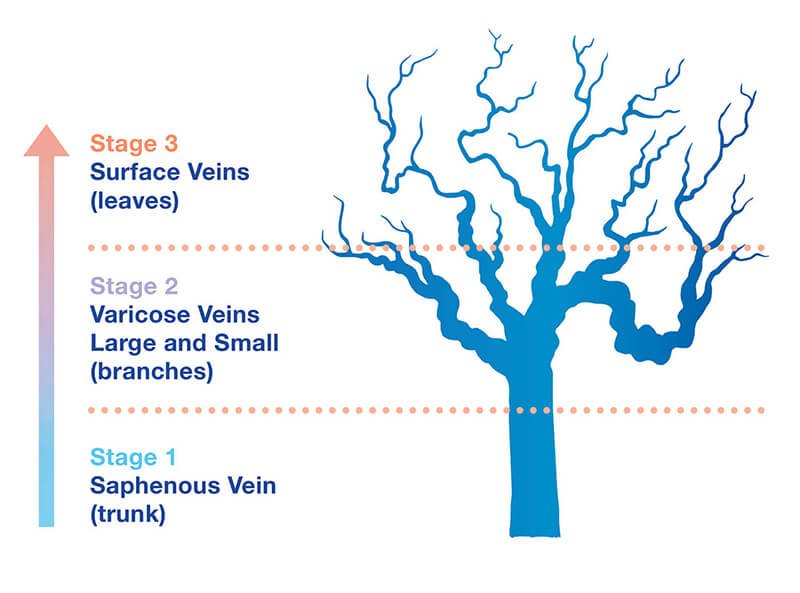
Think of your veins like a tree
Visible on the surface are the leaves and branches, while deep under the skin lies the trunk. This ‘trunk’ supplies blood to the branch vessels and is typically where the problems lie. Our staged approach to treatment means that we solve the underlying malfunction in the trunk first, before moving on to affected branch vessels to improve the aesthetic appearance of bulging varicose veins.
The last step is cosmetic treatment of remaining surface veins. Our primary focus on medical, not cosmetic, treatment gives our patients the best results possible and frees them from the daily discomfort and pain of varicose veins, while improving their confidence at the same time by removing the visible varicosities.
Explore Your Treatment Options
Our Approach to Vein Treatment
Unlike some clinics that focus on treating what they see on the surface, we use an evidence-based “best practice” treatment approach to finding and treating the underlying cause of your vein problems not just the areas of surface cosmetic concern. This approach is typically the opposite of that employed by cosmetic clinics but has been proven to give the best long-term outcomes with the least chance of complications.
We will not treat patients without first performing a detailed “in house” scan to identify any underlying vein issues causing what is seen on the surface.
Highly targeted and advanced ultrasound scanning is essential to getting the correct diagnosis and therefore the appropriate treatment. We do all ultrasound scans “in house” to ensure quality control and maintain our high standards and success rate.
Underlying vein “leaks” and all medically significant vein issues are treated first to ensure the best possible long-term outcome.
Our focus and commitment is to prioritise medically significant vein disease to relieve discomfort, pain and reduced quality of life caused by varicose veins as quickly and painlessly as possible. Once the medical stage of treatment is complete, any residual cosmetic vein issues can then be addressed.
In practice this means that the underlying malfunctioning veins (visible only on ultrasound) are treated first, the larger bulging surface veins next and the small fine non bulging surface veins last.
Why Choose The Vein Clinic Perth
For Your Varicose Veins Treatment
Specialist in Leg Veins
We specialise in the treatment of varicose veins in legs only. This means we are the best at what we do; relieving the symptoms of venous insufficiency. Where other specialists may split their attention over multiple areas, our singular focus means you get the best possible care.
Advanced & Innovative Minimally Invasive Treatments
We provide gold-standard treatments to the people of Perth using the latest technology, and are constantly innovating and developing pioneer methods to improve patient outcomes.
Specialist Diagnosis
Dr Luke Matar brings decades of radiology expertise to his work and oversees the entire diagnostic, treatment, and follow-up process, ensuring the highest quality control possible.
Tailored Treatments
Each treatment plan is individualised to your specific condition and desired outcome. We don't take a "one size fits all" approach to treatment; you'll experience a custom-designed plan to give you the best results.
99.5% Success Rate
99.5% initial closure rate with endovenous laser ablation according to our in-house data, after more than 1,000 endovenous treatments to date. Our closure rate is well above industry standard, due to our meticulous precision and care.
Exceptional Value for Money
We work hard to ensure you get the best possible results from the highest quality treatments to ensure your investment pays back lifelong results. Our work is of the highest standard yet our pricing is competitively positioned within the market.
State of the Art Vein Clinic
Our custom-built, beautifully designed specialty clinic in the heart of Subiaco enables us to perform all diagnostic imaging, treatments, and aftercare under the same roof.
Comprehensive Aftercare
We want your results to last. Our comprehensive aftercare program ensures you're cared for every step of the way, from initial post-treatment follow-up through to annual review to maintain your great results.